Dextrocardia
Dextrocardia is a rare congenital heart defect in which your heart is on the right side of your chest rather than the left. This change to your anatomy doesn’t cause symptoms and it’s not dangerous. But it may occur along with other heart defects or genetic disorders — like situs inversus or heterotaxy syndrome — that need treatment.
What Is Dextrocardia?
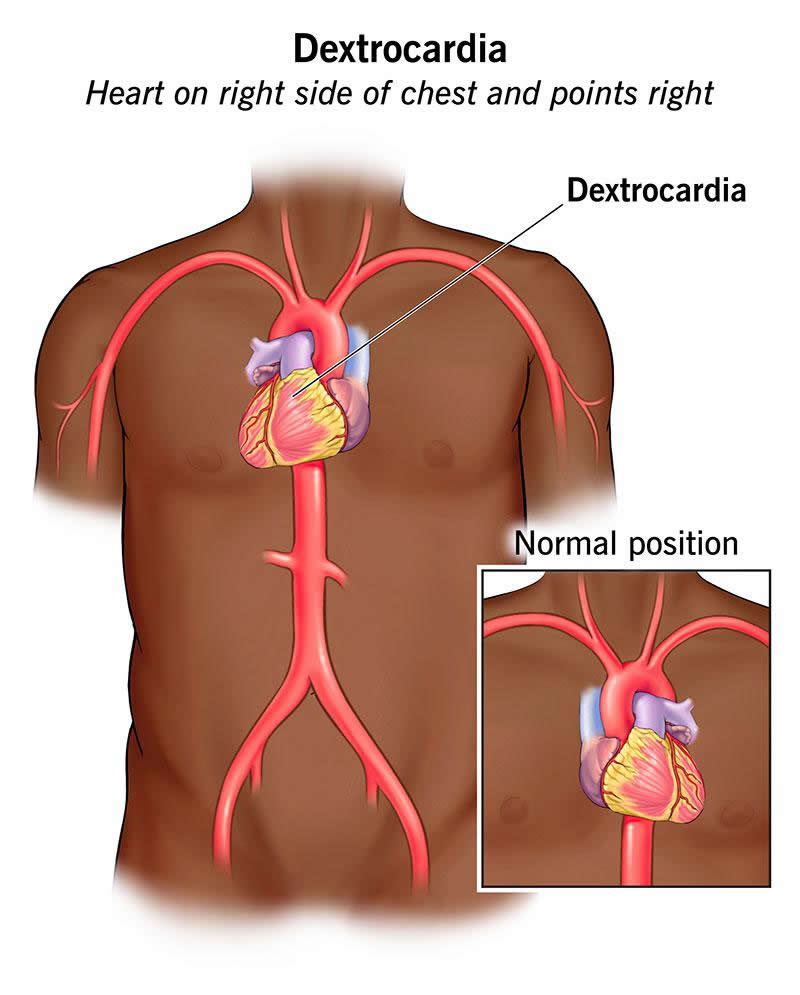
Dextrocardia is a change in how your heart is positioned in your chest. It means your heart is on the right side of your chest and points to the right. This makes it a mirror image of a typical heart. Normally, your heart is on the left side of your chest and points to the left. Dextrocardia is a congenital heart defect, meaning you’re born with it.
On its own, dextrocardia isn’t serious. It doesn’t cause symptoms or complications. And it doesn’t need treatment. But many people with dextrocardia are also born with other conditions. And those conditions may cause problems that need medical attention.
Dextrocardia is rare. It occurs in about 1 in every 12,000 pregnancies.
Types of this condition
Dextrocardia can occur on its own or along with other changes to your anatomy. You might have:
- Isolated dextrocardia. Your heart is flipped from left to right, but all your other organs are arranged normally. You don’t have other heart defects, and your heart functions normally. You won’t have any symptoms.
- Dextrocardia with situs inversus. Your heart is a “mirror image,” but other organs in your chest and belly are flipped, too. Situs inversus can occur as a feature of a genetic disorder called primary ciliary dyskinesia. The disorder causes a range of symptoms from birth.
- Dextrocardia with other congenital heart defects. Many people with dextrocardia also have heart defects that impact their heart function. These defects can cause symptoms and complications that need treatment.
- Dextrocardia with heterotaxy syndrome. This means your heart is a “mirror image,” plus other organs are in unusual positions. Heterotaxy can cause serious problems with organ function.
Symptoms and Causes
Symptoms of dextrocardia
Isolated dextrocardia doesn’t have symptoms. You might not know your heart is on the right side of your chest until you have an imaging test for another reason.
But dextrocardia can occur along with other heart defects or genetic disorders. These conditions often cause the following signs and symptoms — often early in life:
- Extreme tiredness
- Frequent lung or sinus infections
- Getting very tired or out of breath during physical activity
- Irregular heartbeat
- Skin that looks blue
- Skin that looks pale
- Skin and eyes that look yellow
- Trouble breathing or fast breathing
- Trouble gaining weight and growing
- Wet cough
If your child has any of these issues, their provider will do testing to find the cause. Even though dextrocardia doesn’t cause these symptoms, it may show up in the test results.
Dextrocardia causes
Gene changes that happen early in pregnancy cause dextrocardia. More than 60 genes play a role in how your organs are positioned in your body. Researchers are still looking for the specific gene that causes dextrocardia.
About 1 in 4 people with dextrocardia also have primary ciliary dyskinesia. Changes in more than 30 different genes, including DNAI1 and DNAH5, can cause this genetic disorder. Some people can be “carriers.” This means they have a gene change but no signs of the condition.
Diagnosis and Tests
How doctors diagnose this condition
Healthcare providers sometimes diagnose dextrocardia in a developing fetus. They use prenatal ultrasound to check how the fetal heart and other organs are developing. This imaging test may show dextrocardia or other changes in fetal anatomy. Providers may also use a test called a fetal echocardiogram to get a more detailed view of the heart.
But if tests during pregnancy don’t reveal any issues, then a diagnosis might not happen until after birth. Some babies show signs of congenital heart disease soon after birth. This leads providers to run tests to find the problem. But dextrocardia itself doesn’t cause any symptoms. So, children without noticeable heart issues or genetic conditions might not get a dextrocardia diagnosis until years later.
To diagnose dextrocardia in babies, children and adults, providers use a physical exam and testing. During an exam, your provider uses a stethoscope to listen to your heart. A noticeable heartbeat on the right side of your chest can be a sign of dextrocardia.
If providers suspect dextrocardia, they may do more tests, including:
Isolated dextrocardia can show up on these tests — especially an EKG — as an incidental finding. This means that your provider was looking for something else, but the test happened to show dextrocardia.
Associated heart defects
People who receive a dextrocardia diagnosis are often diagnosed with other forms of congenital heart disease at the same time. These include:
- Double inlet left ventricle
- Double outlet right ventricle
- “Hole in the heart” (atrial, ventricular or atrioventricular septal defect)
- Pulmonary atresia
- Pulmonary stenosis
- Tetralogy of Fallot
- Transposition of the great arteries
- Tricuspid atresia
Management and Treatment
How is dextrocardia treated?
Isolated dextrocardia doesn’t need treatment. But it’s important to share this diagnosis with any healthcare providers giving you care. This difference in your anatomy can be helpful for them to know during certain tests and procedures.
If you have dextrocardia along with other heart defects or a genetic disorder, your provider will tailor treatment for those other conditions to your needs. Treatments might include medicines, procedures or surgeries.
Treatment for heart defects — especially severe forms — often happens during childhood. This can be stressful if it’s your child who needs the care. Know that your child’s care team will offer support and guidance. They’ll explain exactly what your child needs. And they’ll help you know how to care for your child at home.
When should I call a healthcare provider?
If your child has dextrocardia, talk with their healthcare provider about what to expect. You may need to look for symptoms related to heart defects or syndromes.
If you have dextrocardia, talk with your healthcare provider about how other conditions may affect your body. Your provider will tell you which symptoms to look for and how to manage them.
Outlook / Prognosis
How long can a person live with dextrocardia?
A person can live with dextrocardia for a long time, but the outlook varies based on other diagnoses. Babies born with isolated dextrocardia (no defects or syndromes) have a normal life expectancy. But babies born with heart defects or genetic syndromes may need treatments or surgeries to manage those conditions. Talk with your healthcare provider about what to expect and the long-term outlook.
A note from Wockr
Dextrocardia is rare, but we’ve learned a lot about it over the years. It was one of the earliest congenital heart changes identified by scientists — all the way back in the 1600s! Today, we know it can occur on its own or as a feature of some genetic disorders. It’s also common for babies with dextrocardia to have other forms of congenital heart disease.
If you or your child has dextrocardia, lean on your healthcare provider for guidance. They’ll explain if there are other issues that need treatment. And be sure to tell all your providers about your unique heart anatomy. They may need to know this detail when taking care of you.