Melioidosis
Melioidosis is an illness you get from the bacterium B. pseudomallei. It lives in soil and surface water, mostly in Southeast Asia and Northern Australia. You can get infected if the bacterium enters through a break in your skin, or if you breathe it in or swallow it. Melioidosis is a life-threatening illness that needs immediate medical care.
Overview
What is melioidosis?
Melioidosis is a disease you get from the bacterium Burkholderia pseudomallei (B. pseudomallei). You get it from direct contact with contaminated soil or water. Its symptoms vary depending on how you got infected and whether you have underlying conditions.
Both humans and animals can get melioidosis, but people can’t get it from animals. Melioidosis is also sometimes called Whitmore’s disease.
Where is melioidosis found?
B. pseudomallei, the bacterium that causes melioidosis, is most commonly found in soil and bodies of water in Northern Australia and Southeast Asia — especially Thailand, Singapore and Malaysia. However, there have been cases of melioidosis all over the world.
In the U.S., B. pseudomallei was found in the environment along the Gulf Coast of Mississippi in 2022. In 2021, the CDC linked a case of melioidosis to an ingredient contaminated with B. pseudomallei in an aromatherapy spray. Three more people, all in different states, got melioidosis from the same contaminated ingredient.
Who does melioidosis affect?
In areas where it’s more commonly found, melioidosis usually affects adults 40 to 60 years old with certain underlying conditions. Children under 15 rarely get melioidosis.
Who is at risk for melioidosis?
You’re at higher risk for melioidosis if you live or work in an area where B. pseudomallei is common and you’re living with:
- Diabetes.
- Alcohol use disorder.
- Chronic kidney disease.
- Chronic lung disease (like cystic fibrosis or COPD).
- Cancer or other conditions that weaken your immune system. HIV doesn’t seem to put you at higher risk of melioidosis.
- Thalassemia.
Jobs or hobbies that put you in contact with soil and surface water (like gardening, landscaping or farming) in areas where B. pseudomallei is common also raise your risk.
Symptoms and Causes
What are the symptoms of melioidosis?
Symptoms of melioidosis depend on where the infection is located in your body. You might have symptoms of infection in your lungs, skin, blood or many places at once.
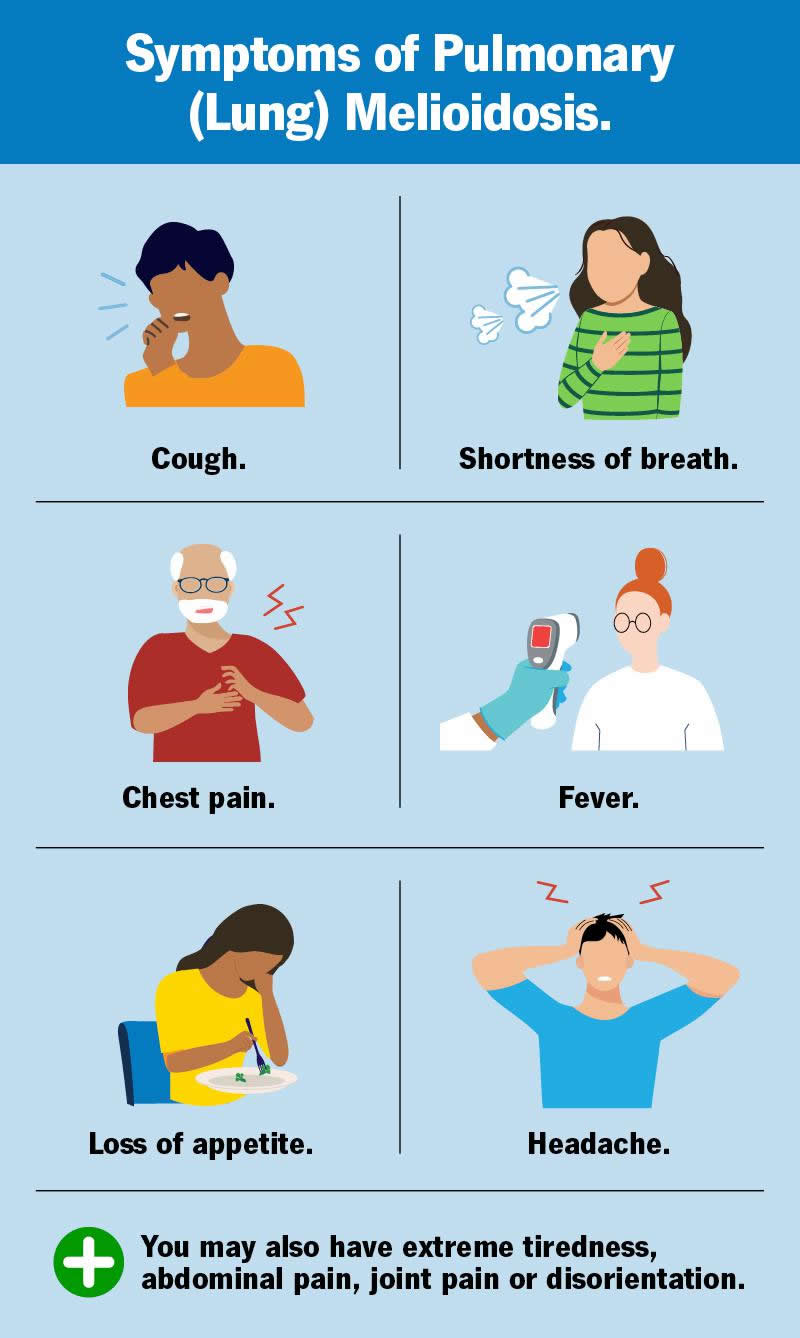
Symptoms of pulmonary melioidosis (melioidosis pneumonia)
If you have melioidosis in your lungs, you might experience:
- Cough.
- Shortness of breath (dyspnea).
- Chest pain.
- Fever.
- Loss of appetite.
- Headache.
Symptoms of melioidosis in your skin
Symptoms of melioidosis in your skin (localized) include:
- Sores, ulcers or abscesses.
- Swollen lymph nodes.
- Fever.
Symptoms of melioidosis in your blood
You may have symptoms of melioidosis in your blood (septicemia) along with skin or lung symptoms. Symptoms of septicemia include:
- High fever.
- Extreme fatigue/tiredness.
- Headache.
- Shortness of breath/trouble breathing.
- Abdominal pain.
- Joint pain.
- Confusion, disorientation or other mental changes.
Symptoms of chronic (disseminated) melioidosis
You might have symptoms of melioidosis that develop over time and last two months or more. During this time, B. pseudomallei can spread to many parts of your body (disseminate). Symptoms of chronic or disseminated melioidosis include:
- Chronic cough.
- Fever.
- Weight loss.
- Night sweats.
- Coughing up blood.
- Stomach or chest pain.
- Muscle or joint pain.
- Headache.
- Seizures.
How long after exposure to melioidosis will I get symptoms?
Most people develop symptoms of melioidosis within one to four weeks of being infected (incubation period). Some cases have happened months or years after exposure to B. pseudomallei.
What causes melioidosis?
The bacterium B. pseudomallei causes melioidosis. It lives in surface water (streams, rivers, lakes) and soil, mostly in tropical or subtropical areas.
How do people get melioidosis?
You get melioidosis from direct contact with water or soil contaminated with B. pseudomallei.
B. pseudomallei can get into your body:
- Through a break in your skin.
- By breathing it in (inhalation).
- By getting contaminated water into your lungs (aspiration).
- By drinking contaminated water or getting it in your mouth (ingestion).
B. pseudomallei infections are more common during rainy seasons or after heavy rainfall.
Can melioidosis spread from human to human?
Person-to-person transmission of melioidosis is rare. The most common way to get infected is through contact with contaminated soil or water.
Diagnosis and Tests
How is melioidosis diagnosed?
To diagnose melioidosis, your healthcare provider will ask you about your symptoms, perform a physical exam and take samples of your blood or other body fluids. They may also ask you about your work, hobbies or travel history.
They’ll send your samples to a lab. There, a technician will use the samples to look for antibodies and try to grow B. pseudomallei. Samples that might be used to confirm melioidosis include:
- Blood.
- Pee (urine).
- Phlegm (sputum).
- Pus from a wound on your skin.
Management and Treatment
How is melioidosis treated?
Healthcare providers treat melioidosis with two phases of broad spectrum antibiotics.
- In the first (intensive) phase, your healthcare provider will give you medicine through an IV (directly into a vein) for at least two weeks.
- In the second (eradication) phase, you’ll take pills for at least three months.
You may need additional types of treatments, like abscess draining, depending on how severe your illness is.
What antibiotics are used to treat melioidosis?
Injected antibiotics your provider might give you include:
- Ceftazidime.
- Meropenem.
- Imipenem.
Oral antibiotics you might take include:
Outlook / Prognosis
What can I expect if I have melioidosis?
Most people who don’t have any underlying conditions and who receive prompt treatment make a full recovery from melioidosis. Treatment can last for months in order to fully get rid of the bacteria. Sometimes your symptoms can come back after you finish treatment (relapse).
The outlook is worse for those who have an underlying condition or who aren’t able to get diagnosed and treated quickly.
Can melioidosis be cured?
Melioidosis can be cured with a two-phase course of antibiotic treatment. However, some infections get severe quickly, and treatment may not be effective in all cases.
Is melioidosis fatal?
With prompt, appropriate treatment, melioidosis is fatal in 10% to 20% of cases. However, the risk of serious illness and death from melioidosis goes up based on:
- Whether or not you have an underlying illness.
- The availability of quality healthcare.
- What organs are affected.
Prevention
How can I prevent melioidosis?
You can reduce your risk of melioidosis, especially in areas where B. pseudomallei is common, by taking a few precautions:
- If you have diabetes or chronic renal disease, avoid contact with soil and standing water.
- Wear waterproof boots when walking in wet soil, pooled water or mud.
- Wear gloves while gardening or working with soil.
- Use waterproof coverings on wounds or sores. Avoid getting water or soil that could be contaminated into wounds.
- Take a shower or wash thoroughly after being in soil or muddy water, or working outdoors.
- Wear a mask that covers your nose and mouth while mowing the lawn, weed whacking or using a high-pressure spray around soil.
- If you think you’ve been exposed to B. pseudomallei, your healthcare provider might recommend taking antibiotics to prevent melioidosis (post-exposure prophylaxis).
Living With
How do I take care of myself with melioidosis?
If you’ve been diagnosed with melioidosis, make sure to take all of your medication as prescribed. If you stop taking antibiotics too soon, you could get sick again.
Keep any follow-up appointments with your healthcare provider. Let them know if your symptoms go away and come back or if you have new or worsening symptoms.
Complications of melioidosis
Melioidosis can spread to most parts of your body and cause complications, including:
- Bone infection (osteomyelitis).
- Joint infection (septic arthritis).
- Collections of pus (abscesses) in your skin, lungs, liver, spleen, brain or other organs.
- Acute respiratory distress syndrome (ARDS).
- Sepsis, a life-threatening response to infection that causes organ damage.
When should I see my healthcare provider?
See your healthcare provider right away if you have symptoms of melioidosis, especially if you live in or have recently traveled to an area with B. pseudomallei. Prompt treatment gives you the best chance for a full recovery.
If you think you’ve been exposed to B. pseudomallei recently, see your provider. They may give you post-exposure prophylaxis — antibiotics that might prevent you from getting melioidosis.
When should I go to the ER?
Go to the ER if you have symptoms of serious illness, including:
- High fever (over 103 F/39.4 C).
- Sudden or severe shortness of breath.
- Severe abdominal (stomach) pain.
- Confusion or other mental changes.
- Chest pain.
- Seizures.
What questions should I ask my healthcare provider?
It may be helpful to ask your healthcare provider the following questions:
- How do I take my medication?
- When should I follow up with you?
- When will I feel better?
- What symptoms should I go to the ER for?
- How can I treat my symptoms at home?
- Am I contagious?
A note from Wockr
Melioidosis is a serious illness that can be difficult to diagnose. That's because its symptoms are similar to those of other, less serious diseases. Melioidosis can be life-threatening if left untreated. If you think you’ve been exposed to B. pseudomallei, have symptoms of melioidosis or are at high risk for severe illness, don’t hesitate to contact your healthcare provider with your concerns.