Tarsorrhaphy
Tarsorrhaphy is a medical treatment that keeps your eyes closed. When used as a treatment, it creates a safe environment that’s ideal for eye healing. It can also be part of efforts to restore facial appearance differences from medical conditions and treatments or injuries. It’s usually temporary but can last from weeks to years.
Overview
What is tarsorrhaphy?
Tarsorrhaphy is a medical procedure that involves keeping your eyes shut for longer periods. Like a cast holds a broken arm or leg in place while it heals, tarsorrhaphy helps hold your eyelids in place. Tarsorrhaphy is usually unilateral, meaning only done on one eye. But your provider can do it on both sides if necessary.
Closing your eyelids can help with several different conditions and issues. But tarsorrhaphy (pronounced “tar-SORE-oh-fee”) is mainly for keeping your eyelids shut to prevent further injuries and issues on your eyes’ surface.
What are the different types of tarsorrhaphy?
Tarsorrhaphy combines two Ancient Greek words that mean “foot” and “to sew.” The “foot,” in this case, is the foot of your eyelid, the lower edge where your upper eyelid can seal against your lower eyelid. And while tarsorrhaphy may involve sewing stitches (sutures) to close your eyelids, there are also several other ways to get the same effect without stitches.
There are a few different factors that your eye care specialist or other provider can consider when deciding which form of tarsorrhaphy can help you best.
How long the closure needs to last
Tarsorrhaphies keep your eyes closed for extended periods. That can mean any of the following:
- Short-term temporary. This refers to tarsorrhaphies that last days or weeks.
- Long-term temporary. Experts may call these “permanent” tarsorrhaphies because they can last for a much longer time, months or even years.
- Permanent. This typically refers to tarsorrhaphies that an eye specialist or other provider can’t easily reverse. This often means tarsorrhaphies that need to last the rest of your life.
The degree of closure
Tarsorrhaphies can vary depending on how much your eye needs to close. Some of the different ways that can work are:
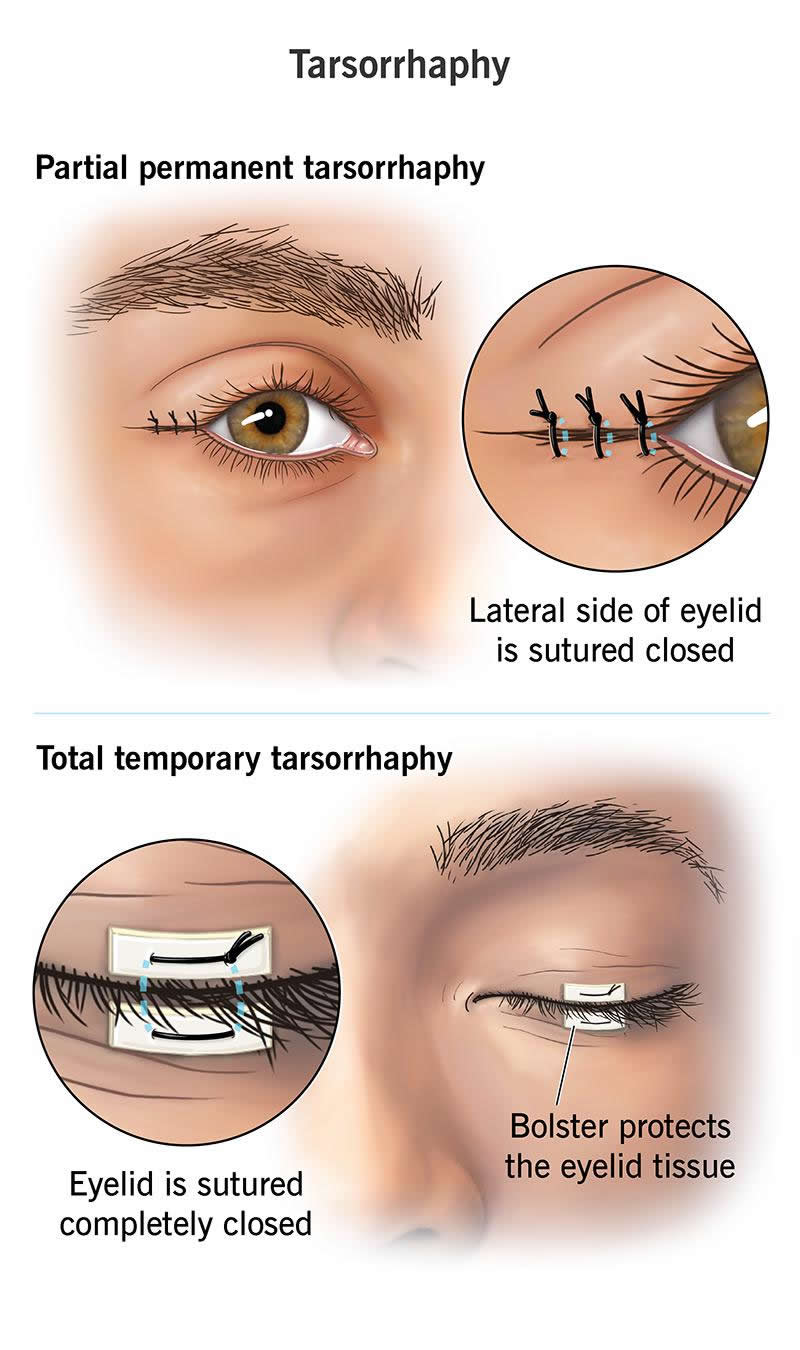
- Partial tarsorrhaphy (lateral tarsorrhaphy). This means your eyelids aren’t completely closed. You can still see through the gap in the middle where they aren’t held together.
- Total tarsorrhaphy. This means sealing your eyelids completely closed.
The method of closure
Tarsorrhaphies can involve a few different methods. They include:
- Tape splints (using adhesive strips to hold your eye shut)
- Cyanoacrylate glues (similar to glue used for minor household repairs but available in medical-grade forms)
- Temporary sutures (the kind your body can absorb)
- Permanent sutures (the kind a healthcare provider will have to remove later)
- OnabotulinumtoxinA (Botox®), which temporarily paralyzes the muscles you use to open your eye
- Surgery (this can involve sutures only or taking skin from other places and using it to close the palpebral fissure permanently)
Why is tarsorrhaphy done?
Tarsorrhaphy has several uses. Sometimes, it’s a treatment for a condition or issue that already happened. Other times, it’s a preventive measure to avoid future complications.
Eye surface diseases and injuries
Tarsorrhaphy can be a very helpful treatment when you have a condition that affects your eye surface or are at risk for eye surface issues. Examples include:
- Conditions that cause incomplete eyelid closure. Conditions like Bell’s palsy may disrupt eyelid closure.
- Long-term sedation with mechanical ventilation. People who can’t close their eyes completely have a much greater risk of damage to their corneal surface.
- Exposure keratitis. This is eye inflammation and damage from being exposed to air and/or harsh temperatures for too long. This is more likely with incomplete eyelid closure or eyelid weakness.
- Corneal burns. This includes thermal (heat) burns and chemical burns.
- Corneal diseases. Examples include corneal dystrophies, injuries or infections. It also includes treatments for corneal infections.
- Nerve-damaging cornea disease (neurotrophic keratitis). This is dangerous because it means your cornea can’t feel irritants or foreign objects, making it more vulnerable to damage.
- Recurrent corneal erosions and other types of keratitis. These may need tarsorrhaphy when they don’t heal properly or quickly.
- Preventing swelling (chemosis). This condition can affect the white of your eye, the sclera, after an eye injury or eye surgery.
Conditions that affect eyeball shape or position
If your eye shape or position changes, it can be harder to close your eyes properly. Not being able to close one or both eyes is called lagophthalmos (pronounced “lag-op-ff-THALM-oh-ss”). Conditions that can cause this include:
- Bulging eyes (proptosis)
- Eye cancers and tumors in and around the eye that change its shape or position
- Graves’ disease and thyroid eye disease
- Severe eye conditions or injuries that result in partial eye removal (evisceration) or total eye loss (enucleation)
Eyelid conditions, injuries or surgery
Conditions that affect your eyelid movement, placement or control can affect how your eyes close. Examples of these conditions include:
- Floppy eyelid syndrome
- Facial paralysis conditions, including Bell’s palsy, Moebius syndrome or damage to your facial nerve
- Eyelids that turn outward too much (ectropion), keeping them from sealing shut properly
- Conditions that affect consciousness or make a person blink less often, like a coma from a severe head injury
Risks / Benefits
What are the advantages of tarsorrhaphy?
Tarsorrhaphy has a number of advantages:
- There are many different ways to do it
- It has a very high success rate for healing eye issues (between 80% and 100%)
- It can be a preventive treatment, helping avoid more serious or permanent damage
- It’s possible to do the procedure so it lasts months or even years
- Most of the ways to do it are reversible
What are the disadvantages of tarsorrhaphy?
Tarsorrhaphy has a few disadvantages or reasons why it might not help. They include:
- You shouldn’t drive after tarsorrhaphy until your ophthalmologist says it’s OK.
- Some of the methods, like tapes or cyanoacrylate glues, can irritate your skin.
- You won't be able to see normally in part of your field of view while your eye is shut (the amount of decreased vision depends on whether the tarsorrhaphy is partial or total and the exact method used).
- The surgery methods come with the same possible complications as any surgery, like pain, bleeding and infection.
Recovery and Outlook
How soon after tarsorrhaphy will I feel better?
If tarsorrhaphy involves sutures or surgery, your eye care specialist or other provider will use topical medications to numb your skin so the procedure doesn’t hurt. After the procedure, your specialist may prescribe medications for pain. But you may not need any medications or may only need over-the-counter medications like acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs).
Your eye specialist or other provider can tell you more about what to expect and how to manage any pain or discomfort.
In cases where tarsorrhaphy should be temporary, the time it’ll last can vary. Your eye care specialist will tell you if they need to do follow-up checks to assess your eye health and recovery. Those follow-ups will be key in determining if and when to reverse the tarsorrhaphy and let you go back to using the affected eye.
How can I take care of myself after tarsorrhaphy?
After tarsorrhaphy, there are some important things you can do to help your odds of a favorable outcome.
- Don’t rub your eyes. Doing so can disrupt eye healing and be very unpleasant or painful. Your eye care specialist can teach you how exactly to deal with any itching that occurs on or around your eyelid.
- Follow the instructions from your eye care specialist (or other provider) exactly. It’s common after tarsorrhaphy with sutures to need to wear an eye shield or other protective piece to keep things from touching your eye or eyelid.
- See your eye care specialist as recommended. Follow-up visits are a crucial part of making sure you get the full benefits of tarsorrhaphy.
When should I see my healthcare provider?
In addition to seeing your provider as recommended, you should call or see your provider if you notice any of the following:
- Loosening or tearing of the stitches, including any related injury to the surrounding skin
- Changes in your vision
- New symptoms affecting your eye, eyelid or the skin around your eye
- Swelling, redness, oozing or discharge, or pain around the eyelid closed using tarsorrhaphy
A note from Wockr
Having tarsorrhaphy to keep one or both eyes shut isn’t something anyone wants, and facing that possibility can be scary or frustrating. But one reason why this procedure is an important treatment option is because it has an extremely high success rate. It can also help with many conditions and issues. Your eye care specialist or other provider can explain if tarsorrhaphy is likely to help and the options they recommend for your specific case and needs.